|
Author: Ana Norio Bran 2020 proved to be the year of many changes in the lives of so many people. Having to deal with a global pandemic was a tough situation for essential workers, children, and families. With so much uncertainty in the world, it became easier for many people to feel alone and isolated, with no one to turn to. As a result, there has been a negative impact on people’s mental health suffering from different stressors. People are understanding that to get through such a difficult period, putting their mental health first is the key. So what are people doing to improve their mental health in these times of crisis? The answer is simple - therapy. Misconceptions of Therapy When the idea of therapy comes to mind, some people still have a response shaped by stigma, thinking that you have to be “crazy” or “weak” to need therapy and that because you can’t fix it on your own, there might be something “wrong” with you. This thinking leads to fear and shame around seeking help. When the idea of therapy comes into someone’s mind, it can sometimes be seen as a scary thing. “Am I crazy?” or “Is there something wrong with me?” can be the first questions someone may ask themselves when considering seeking therapy. There can often be a societal stigma associated with having or acknowledging one’s mental health issues, and some may feel that they are considered “atypical” to society. When addressing one’s mental health it is viewed as a deviation from societal norms, people might feel ashamed for the way they are feeling, which prevents them from seeking professional help. Thankfully, attitudes towards mental health are changing for the better in today’s society. In a study conducted by the National Alliance of Mental Health, researchers found that 20.6% of individuals experience mental illness like anxiety and stressors of everyday life. While the prevalence of these issues has seen a steady increase since 2019, it has shown that only 1 in 20 people experience severe mental health issues. The misconception that only people with severe mental health issues can seek therapy is something that limits people from seeking help, but thankfully, we have seen that stigma being broken down. While therapy is known to target these specific areas, it also works with individuals suffering from anxiety and uncertainty, which many are experiencing in today’s climate. When increasing numbers of Coronavirus cases were first being published, people were reporting a negative effect on their mental health caused by anxiety and stresses of the world. Kaiser conducted a study in the United States in March of 2020, which found that 32% of people at the start of the lockdown were worried about their mental health, and within a week, it rose to 45%. This rise was due to many different issues including the future of current jobs, economic impact, and risk of exposure to Covid-19. These issues have shown individuals that they are not the only one’s dealing with these anxieties and uncertainties, many are in the same position. The pandemic has shown many people the importance of therapy and shown them that there is help. What is Therapy? Dr. Ryan Howes, Ph.D., ABPP, a clinical psychologist in California is an advocate for debunking misconceptions of what therapy entails. Seeking therapy can be used to improve your everyday life. Therapists use different techniques to better understand their clients to provide the best solutions to their problems. Therapy offers opportunities to self-reflect, and often the therapist will work alongside the client to come up with ways in which one can live a healthier and more productive lifestyle. Especially within this current global pandemic, therapists provide their skills to help clients with managing stressors of life and cope with the overwhelming amount of uncertainty they might have. Because there are numerous reasons why someone might want to consider therapy, there are different theoretical approaches that a therapist may use. Some of these include but are not limited to:
Depending on the reasons why someone is seeking therapy, the individual may want to do their research to determine which of these approaches (or others) may be the best fit for them. Although therapy where you lie on the couch, talk about your childhood and mother is still what some therapists do, and some are just there for a supportive ear, many therapists are focused on helping you to make changes to achieve your goals in the present, helping you overcome difficulties, and strengthen relationships in your life, so that you have others to turn to, rather than staying in therapy for years. Many providers will have a website or information listed about their approach online, where potential clients may learn more about their practice and find the therapist that is the right fit for their issues and goals. Therapy in Today’s Climate Most therapists have been working from home during the pandemic, which is one reason why teletherapy has become very popular. Teletherapy is remote therapy that is done through the use of technology to receive counseling in areas of an individual’s choice. This form of therapy is done in many ways including, by phone, messaging, and the most used to date, video-conferencing. Individuals are finding that this allows them to remain socially distanced but also stay connected virtually. There has been a sharp increase in remote therapies that are being offered remotely for individuals to get help and feel heard. While some consumers may be skeptical that remote therapy is as good as in person therapy, research has found that it is just as effective as in person. In a 2013 review in the Telemedicine Journal and E-Health, researchers found that video-conferencing therapy was just as effective for most parameters, like feasibility, outcomes, age, and satisfaction, which has continued to grow since then. Online therapy has shown many benefits including flexibility, convenience, affordability, and same confidentiality as with in person. Individuals can schedule a time that works best with their schedules to meet with a therapist without having to leave their homes. This gives therapists the chance to see individuals in a more comfortable environment and get a sense of who they are outside of an office setting. Research has also found that individuals are more likely to seek out remote therapy because of the affordable costs. With having to drive to and from the therapist’s office, the costs were higher for clients but now that there is a remote option, individuals are finding it easier to get a consultation at a cheaper price. As some therapists are going back to the office, they are finding that many of their clients are wanting to stay online because it is so convenient. It is important to remember that you don’t have to deal with your struggles alone. Licensed therapists are available and want to help you. Through therapy, it is important to discuss everything you might be going through and what you may feel comfortable sharing. By being open and willing to share, professionals will help you tackle them head-on through the therapy that best fits. Remote therapy is providing a greater opportunity for individuals to seek out professionals especially during the Covid-19 pandemic. Therapists are wanting to help you in any area that you might need counseling in and guide you through the whole process. Whether it is by phone, messaging, or video-conferencing, remote therapy is available to those wanting the opportunity to seek help. Sources: https://www.kff.org/health-reform/report/kff-health-tracking-poll-early-april-2020/ https://www.cdc.gov/coronavirus/2019-ncov/daily-life-coping/reducing-stigma.html https://www.apa.org/topics/therapy/psychotherapy-approaches https://www.nhsinform.scot/tests-and-treatments/counselling-and-therapies/psychotherapy https://www.nami.org/mhstats https://www.apa.org/ptsd-guideline/patients-and-families/cognitive-behavioral https://www.apa.org/news/press/releases/2010/01/psychodynamic-therapy https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3662387/
4 Comments
Author: IAP Staff In April of 2021, the Centers for Disease Control and Prevention (CDC) declared that racism is a threat to public health in the United States. COVID-19 has re-illuminated that reality across the country in both the physical and mental health consequences of the pandemic. Communities of color have experienced a disproportionate number of COVID-19 cases, deaths, and mental illnesses during the pandemic. While the specific reasonings are layered, they are rooted in the United States’ historical systemic racism that the CDC warns of. In addition to disparities in access to quality preventive health care and treatment, racism has also fueled a deep-seated distrust of healthcare systems and governmental systems more broadly in many communities of color.
A few notable examples of medical racism throughout U.S. history include James Marion Sims, who has been called “The Father of Modern Gynecology” in the United States and was known to have come to many of his surgical learnings by experimenting on enslaved Black women without anesthesia or consent.[ii] Recent news reports have revealed what was already widely known throughout Native communities about atrocities and deaths that occurred at government-funded “residential schools” for Native youth throughout Canada and the United States.[iii] In the 1950s, physicians and researchers at Johns Hopkins University took the cells of a Black patient, Henrietta Lacks, without her knowledge or consent when she was being treated for cervical cancer and used them for decades following her death in the development of many medical advancements.[iv] All of these and the countless other known and unknown examples of institutionalized and medical racism throughout the history of the United States have resulted in an understandable distrust of American health systems amongst communities of color that continues through the present day. The pervasiveness and complexities around such racialized traumas [v] cannot be understated. We are seeing the consequences of such being repeated during the current pandemic with higher numbers of cases and deaths in communities of color.[vi] The mental health implications of the various stressors resulting from the COVID-19 global pandemic is no exception to this pattern of racial disparities in the United States. For so many people across the country, the life changes that resulted from the pandemic brought on new or more severe mental health challenges. In fact, it would likely be difficult to find many people whose mental health has not been impacted in some way -- big or small -- over the duration of the ongoing pandemic. Given the novelty of the circumstances stemming from the pandemic in modern times, the depths of the full mental health implications will take years for researchers to understand. However, initial studies already show increases in anxiety, depression, and other mental health issues. For example, a January 2021 survey by the U.S. Census Bureau found that four out of ten adults in the United States reported symptoms of anxiety or depression, compared to one out of ten adults who reported those symptoms prior to the pandemic in January through June 2019.[vii] Researchers are of course continuing to track these issues, but not surprisingly, initial studies have also found racial disparities in mental health challenges during the pandemic consistent with the CDC’s determination that racism poses a severe threat to public health in the United States.[ix] Some states, including Maryland and Connecticut, have reported disproportionate increases in suicide rates among Black residents during the early months of the pandemic.[x] In Maryland, suicide rates for Black residents doubled while rates for White residents dropped by half. Stressors such as job loss, food insecurity, deaths of loved ones, and disruptions to access to support services have disproportionately impacted people and communities of color throughout the pandemic.[xi] One survey published by the CDC found that Latinx adults reported higher levels of stress related to not having enough food or stable housing than did U.S. adults in other racial and ethnic groups.[xii] All of these stressors are compounded by the heightened racial stress for people of color during 2020-21, including increased attention to and pushback on racial violence from law enforcement agencies, shifts in immigration policies, and increases in racist violence against Asian Americans and Pacific Islanders throughout the pandemic, among others. Increased access to quality mental health treatment for people of color who have been disproportionately impacted by the various stressors of the COVID-19 pandemic will be an essential part of the collective recovery process for the nation. The CDC and other organizations have taken initial steps towards providing resources to increase awareness and accessibility. These issues are certainly challenging, but it is incumbent upon mental health practitioners to do their part by learning more about the issues, educating themselves on the cultural and historical context of race in this country, and ensuring that their services are culturally-informed. There is a steep hill to climb with mental health recovery from the COVID-19 pandemic, but any such efforts will be insufficient without attention to these issues. For additional information, please see the resources listed below and cited at the end of this post. Sources ● CDC: Racism and Health Information ● Mental Health America: BIPOC and LGBTQ+ COVID-19 Resources
[i] https://www.cdc.gov/media/releases/2021/s0408-racism-health.html [ii]https://www.history.com/news/the-father-of-modern-gynecology-performed-shocking-experiments-on-slaves [iii]https://www.usatoday.com/story/news/nation/2021/05/30/native-american-boarding-schools-abused-neglected-thousands-us/5263769001/ [iv] https://www.smithsonianmag.com/science-nature/henrietta-lacks-immortal-cells-6421299/ [v] https://www.mhanational.org/racial-trauma [vi] https://mhanational.org/bipoc-communities-and-covid-19 [vii]https://www.kff.org/coronavirus-covid-19/issue-brief/the-implications-of-covid-19-for-mental-health-and-substance-use/ [viii]https://www.nimh.nih.gov/about/director/messages/2021/one-year-in-covid-19-and-mental-health [ix]https://www.hsph.harvard.edu/news/multimedia-article/covid-19-brings-persistent-racial-and-ethnic-disparities-to-focus-implications-for-population-mental-health/ [x] https://www.statnews.com/2021/05/07/as-the-covid-19-crisis-ebbs-in-the-u-s-experts-brace-for-a-long-term-impact-on-mental-health/ [xi]https://www.psychiatrictimes.com/view/mental-health-disparities-among-black-americans-during-covid-19-pandemic [xii] https://www.cdc.gov/mmwr/volumes/70/wr/mm7005a3.htm Author: Marisol Caldera Have you ever felt nervous about asking someone a favor? Do you tend to fear the outcome you will experience if someone says “no”? The way we socialize is all due to a phenomenon in social psychology called egocentric bias. When we ask others for favors, some people can become stressed out and often feel anxious because we believe others will decline our requests. This then prevents us from making social interactions with others, as we are afraid of being rejected or judged. This is a completely normal experience, as almost every person is taking a risk when trying to ask others for a simple favor or task. Egocentric bias plays an influential role in our social tendencies because it keeps the focus more on your perception instead of the other people you are interacting with while in a social situation. Imagine ordering your favorite dish at a restaurant, but they end up getting your order completely wrong. You want to ask the waiter to take the dish back to the chef and bring what you had originally asked for, but you are too nervous to ask the server to fix the dish because you believe they will say “no”. This is an example of your egocentric bias taking over in social interaction. You cannot perform the simple task of asking for the correct dish because you are more afraid of how the waiter will react to your request. This unveils how effortlessly and impactful egocentric bias can play a part in the simplest tasks that take place in your everyday life. In the podcast, “The Influence You Have: Why We Fail to See Our Power Over Others,” Vanessa Bohns, a professor of Organizational Behavior at Cornell University, explains her extensive research on egocentric bias. In her work, Professor Bohns will typically begin an experiment by asking her research assistants how many people they expect to comply with their experiment before their research begins, and the results were shocking. In one particular experiment, Professor Bohns requests her research assistants to ask strangers if they could agree to go along with an unethical task. The task consisted of asking people to vandalize library books and writing the word “pickle” onto the pages. The participants in the study hypothesized that only 28% of the people they solicited would agree to the immoral requests. After the experiment, data revealed that 64% of the people who were asked to vandalize the library books ended up agreeing to do so. This actively demonstrates that we tend to underestimate who will comply with our requests, thus triggering our egocentric bias. We automatically assume that people will react negatively to our requests, which causes us to feel anxious when in reality, they are more likely to say “yes” than we realize. What we do not realize is that egocentric bias limits the consideration we have of other people's points of view. We fail to see how the other person in a social interaction feels. To give you an idea, imagine the point of view of a waiter at a restaurant. Part of the waiter’s job is to be concerned about your experience and they want you to let them know if there is an issue with your order. Egocentric bias blinds your perspective, making it easy to assume that others will react negatively, while that may not be the case - and in fact, that may just be a projection coming from within ourselves and our own insecurities. Due to social norms, we tend to feel uncomfortable when saying “no” to others, making it less likely for your waiter to decline your request. People want to be viewed as good, so when we say “no” we start to feel guilt. Our egocentric bias makes us focus on our guilt, thus making us agree to tasks. Some may know this experience as “guilt-tripping”. In reality, both you and your waiter are being affected by your own egocentric bias. Next time you want to ask someone for a favor and you are too afraid, just take a few deep breaths, and ask. Most likely the person will say yes, as they might feel more willing to comply because they feel the need to help others. Some people will even agree just because they want to look like a good person in front of society. Supposing that you still do not feel comfortable asking someone for their assistance, you may want to take into account how the other person might feel. If you hold back on asking a favor, due to your concern of being rejected, you will never know the outcome. That person might have been more willing to go along with your request than you realize. Do not underestimate the influence you have on others as their answer may be surprising. You hold more power than you think. Sources: Vedantam, Shankar et al. “The Influence You Have: Why We Fail to See Our Power Over Others.” Hidden Brain A Conversation About Life’s Unseen Patterns, NPR, 24 February 2020,https://www.npr.org/2020/02/20/807758704/the-influence-you-have-why-were-blind-to-our-power-over-others
How the Triangular Theory of Love Can Lead to Fulfilling Intimate Connections and Relationships7/23/2021 Author: Alejandra Hilbert 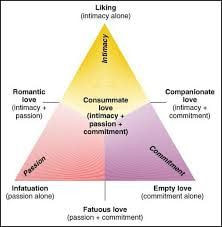 Psychologist Robert Sternberg proposed that there are three different building blocks which combine to form different types of love. These components are intimacy, passion, and commitment. Intimacy is defined as feelings of warmth, understanding, trust, support, and sharing. Passion is characterized by physical arousal and desire, excitement, and need. Finally, commitment is typified by feelings of permanence, stability, and the decisions to devote oneself to a relationship and to work to maintain it. Under Sternberg’s model, there are eight relationship types (as illustrated here). Utilizing Sternberg’s conceptualization of romantic partnerships, one can compare a romantic relationship to a stool. A stool only propped up by one leg is much less likely to support one’s weight, whereas a three legged stool could unwaveringly; thus, relationships with two or more of the critical components will lead to a greater sense of fulfillment, dependence, and security. Utilizing the stool metaphor, single leg relationships are those with only one building block. An example of this relationship structure is empty love, which describes a relationship where commitment is high, but there is little intimacy or passion—in essence, a work relationship. Conversely, a relationship which is high in passion but lacks intimacy and commitment is infatuation, or colloquially known as a crush. Intimacy, passion, and commitment are all absent in nonlove. Ideally, a strong dose of all three components should exist within the partnership, as typified by consummate love. Throughout the course of the relationship, there will likely be a shift in prevalence of particular blocks and how they appear. Passion may run high in the beginning of a new romantic relationship, as coined by the term new relationship energy (NRE). Sheer novelty adds excitement and energy to new loves. Once a relationship is established and novelty is lost, passion slowly subsides; typically the longer a relationship lasts, the less passionate it becomes. However, other components, like intimacy and commitment, are bolstered to maintain balance. Time alone does not cause intimacy, passion, and commitment to occur and grow, but rather deliberate effort is needed to foster these critical components if they do not initially exist in your partnership. Knowledge of this model of love may help couples avoid pitfalls in their relationship, allow for intentional work in areas that need improvement, or aid partnerships recognize when it may be time for a relationship to end. Sternberg asserts that reaching consummate love is often easier than maintaining it. Understanding that there is an ebb and flow in which building blocks may appear in our relationships, have are few recommendations on how to cultivate continuous consummate love:
Sources
Author: Cate Cabri Connections with others have a major impact on our happiness as well as our well-being. One way that many people seek to strengthen these connections with others is through the use of social media. Social media has become so commonly used in our society as a main method of communication for many people, sometimes even replacing face-to-face interactions. Although there are some positive aspects of using social media, there are also major concerns, including raising levels of anxiety and depression. If used in an unhealthy way, social media can take a major toll on people's mental health. A few warning signs to look out for that social media could be negatively affecting your mental health include:
However, if used in a healthy way, there are many positive aspects of social media.
Research on the impacts of social media on anxiety has shown that anxious people tend to rely on social media as a means of escaping from what they are worried about. However, once on social media, new stressors become an issue that fuels the initial anxiety that the person was already experiencing. Individuals with Generalized Anxiety Disorder, for example, often compare themselves negatively with others on social media, which leads to a higher level of anxiety than they were initially experiencing. Social media can be an addictive platform. Research has shown that posting a photo and getting lots of likes and positive, validating comments can be addictive. When you receive positive feedback on a post, this triggers the release of dopamine in the brain (a “reward” chemical). This can cause people to want to continue posting to get more of this validation. This is something to keep in mind when using social media - what is your intention and why are you choosing to post? There is not necessarily one correct intention with posting on social media but it is something to consider, as using social media for the wrong reasons (like for the purpose of only using it to try to get validation or trying to fit in with others) can lead to an unhealthy relationship with social media and can contribute to feelings of anxiety and depression. Overall, there are positive aspects to social media when used in a healthy way, and it is important to consider your own social media use and how it is affecting your life. Check in with yourself on your social media use and consider any adjustments that you could make to ensure that social media is affecting your life in a positive way. Sources: Social Media and Mental Health The Impact of Social Media on Youth Mental Health Anxiety and Social Media Use Does Social Media Cause Depression?  About the author: Cate is a student at Loyola University Chicago where she is majoring in Psychology with a minor in Psychology of Crime and Justice. She plans on attending graduate school to become a clinical social worker. In her free time, she enjoys hiking and spending time with family and friends. Author: Katie Borrman My work friends and I were all freshly vaccinated and looked forward to having another dinner party together after a year of isolation. Most of us had kept to our “pods” (a limited group of friends/family to socialize with during the pandemic), and hadn’t risked socializing outside of that. It was the first time in a year I expanded my social circle to an indoor party with friends in different pods. I was excited. What I didn’t expect was to feel an inescapable level of anxiety. I remember feeling like I was watching myself in the group, asking myself, “Why aren’t you talking more? Why are you so tired? Do they think you’re not having fun? Do they think you have changed during this year of isolation? Have I changed for the worse? Do you have anything to contribute? Why are you being so boring? Does anyone else feel like the volume is too high?” This anxiety-induced questioning led me to a full bodily shutdown, and I felt paralyzed. The last thing I expected during this reunion was for me to excuse myself at 9:00 pm to read a book and fall asleep before anyone else. After this event, I tried my hardest not to judge myself, and instead, evaluate psychologically what was going on. The DSM-V describes social anxiety disorder with 10 main criteria, but for my situation, the first 3 criteria pertain the most directly:
These symptoms checked out with how I was feeling at the reunion. Social anxiety had never been a controlling element in my life, and I knew that the Covid-19 lockdown was a major contributor to this psychological state. As a society, we are going through something difficult, unpredictable, and traumatic. According to the Center for Disease Control and Prevention (CDC), “Elevated levels of adverse mental health conditions, substance use, and suicidal ideation were reported by adults in the United States in June 2020. The prevalence of symptoms of anxiety disorder was approximately three times those reported in the second quarter of 2019 (25.5% versus 8.1%).” Whether or not you have had experiences with social anxiety before, or are recently feeling its crippling effects, there are many reasons why an increase in this type of unhelpful habit of thinking may have developed over the past year: Expectations for personal growth during lockdown Lockdown brought about many opportunities for people to explore new interests, pick up old hobbies, or “reset” their bodies in a way that was not afforded to them while working full-time. It’s hard not to compare your own personal growth to those who share their experiences freely on social media. But not all experiences during lockdown are seemingly “self-enhancing.” According to the American Psychological Association’s Stress in America Report, since the pandemic started: 61% of adults reported experiencing undesired weight changes, nearly 1 in 4 adults reported drinking more alcohol to cope with their stress, nearly half of Americans said they delayed or canceled health care services, essential workers were more than twice as likely as nonessential workers to have been diagnosed with a mental health disorder, and Gen Z adults were the most likely generation to say that their mental health has worsened. Those dealing with social anxiety might fall victim to an illusion of unworthiness, or a cycle of thinking that minimizes their own experience. If this thinking has dominated your thoughts during the lockdown, then assimilating back into social circles face-to-face might bring about the same negative cycles of thinking - that your own experience is inadequate, disappointing, or depressing compared to those around you. Conflicting media information There are endless amounts of information one can digest through media outlets pertaining to Covid-19, and after a year of deciphering which information feels the most accurate, we are bound to come into conflicting points of view on the safety, regulation, and validity of the information we are taking as truth. The CDC has methods for tracking the deaths, outbreaks, and hospitalizations of Covid-19, as well as which public health measures seem to be working. However, according to the CDC, “...counting exact numbers of COVID-19 cases is not possible because COVID-19 can cause mild illness, symptoms might not appear immediately, there are delays in reporting and testing, not everyone who is infected gets tested or seeks medical care, and there are differences in how completely states and territories report their cases.” This ambiguity can cause tension within our community and social circles due to a lack of consensus and trust. These disagreements can turn into confrontation or avoidance, and in turn, exacerbate anxiety levels while socializing with new or familiar groups. Grief, loss, and survivor’s guilt For anyone grieving the loss of loved ones close to them, or feeling loss and grief on a “global community” scale, reemerging from lockdown can feel emotionally overwhelming. According to the CDC, “...the prevalence of depressive disorder was approximately four times that reported in the second quarter of 2019 (24.3% versus 6.5%)”. Depression almost always contributes to anxiety levels, and after a year of isolation and social distancing, the question of how to reintegrate can feel nearly impossible to answer. The pressure to “reopen” may feel like too much too soon, and it’s important to let the phases of grief happen naturally and at whatever timeline feels right. Unwillingness to return to “normal” The “reopening” of our community structures is a relief for some, while for others creates a sense of dread. For some, this time in lockdown has given a much-needed dose of self-reflection and an opportunity to change personal circumstances and values. For others, reopening might feel simply unsafe. According to the APA Stress in America Report, when asked about feelings concerning the future, “...more than half said they feel uneasy about adjusting to in-person interaction once the pandemic ends (57% Black, 51% Asian, 50% Hispanic and 47% white).” The pressure to return to whatever “normal” was for us pre-pandemic might feel unaligned. I think the pressure becomes particularly more intense when our usual socializing habits have changed over the course of lockdown. Whether that be switching your social scene completely or having new boundaries around the time you spend socially, a new way of being can cause a lot of anxiety when confronting your peers. These are only a few of the endless reasons why we may be facing social anxiety at this point in a major world transition. It might be hard to end cycles of negative thinking that are based on realistic responses to a global pandemic; so the question of how to manage this type of anxiety can be tricky to relieve. Acceptance Commitment Therapy (ACT) has the goal of adjusting the language we use in talking to ourselves about our anxiety. This method is not trying to eliminate the symptoms themselves - which oftentimes creates more of a problem as the more you try to get rid of it, the worse it can become - but rather manage the anxiety through acceptance, mindfulness, and committed action based on our personal values. This means going towards one’s values, despite the anxiety, rather than waiting to overcome the anxiety to move in the direction of your values. Acceptance Commitment Therapy The first step in this therapeutic process is Cognitive Defusion. The goal of this technique is to separate yourself from the personal sensations, (such as thoughts, feelings, images, and memories), that send anxiety down a self-deprecating spiral; to create space between our private experiences and the reactionary impulse of having judgments and trying to control them. A huge component of this technique is accepting that thoughts of pain and suffering inevitably happen. Trying to eliminate them is like swimming upstream - the harder you try to control them the more the anxiety will build. Ways to practice cognitive defusion are by the use of labeling thoughts as they pop up into your mind. For example, the thought I had at the reunion, “I am being boring”, could have instead been phrased as, “I am having the thought that I am being boring.” In this way, we are becoming mindful of the “judgment” aspect of the thought, without trying to eliminate the thought from happening. Instead, we are acknowledging that it is a thought, as opposed to an objective truth. The second step is Acceptance. Letting unpleasant emotions come and go without resistance is a key factor in this therapeutic process. When we notice the anxiety emerge, we have a choice. We can let ourselves feel it - meaning we can let the anxiety be noticed, remaining in a state of curiosity. The other, more automatic, choice is having an anxious response to the experience of anxiety (i.e. having anxiety about having anxiety). This can be seen as the panic that follows social anxiety, focusing on your future actions, perceptions of others, and shaming oneself into a deeper level of discomfort (also known as “secondary emotions”). Meditative imagery is a useful tool in the acceptance process - imagining the anxious feelings being invited to sit down to tea with you; it can be there, without having to engage or push it away. The third step is Mindfulness. Being in contact with the present moment is at the heart of Acceptance Commitment Therapy. It is necessary to be in a state of mindfulness to achieve acceptance and cognitive defusion. Remaining present will help you not become lost in your thoughts, and will help heighten your level of awareness around the secondary emotions that emerge during episodes of social anxiety. The most simple and effective tool for mindfulness is breathwork. Paying attention to your breath keeps your body regulated and fixated on the present moment. The fourth step is establishing your Values. Affirming oneself in their values builds a strong emotional foundation. From this foundation, one can feel confident and assured in situations that might shake their emotional stability. By reverting to our values we can feel assured that our actions align with our emotional goals and commitments. In my situation, my value was to be connected with my friends and our community. Rather than going to the other room and going to bed early, I chose to stay with them, despite the anxiety and the anxious thoughts, and chose to instead be present with them and my experience. And finally, Taking Action is the last step. Once one’s values are established, it becomes easier to take steps toward fulfilling goals. For people with symptoms of social anxiety disorder, those goals might be something like, “I want to reach out to someone I haven’t spent much time with”, or “I want to call a friend who lives in a different city”, or “I want to make sure I’m giving myself enough alone time, so I won’t feel drained in social situations.” Whatever the “action plan” is, the important thing is to keep the plan aligned with one’s values. Conclusion I tried to recall the feeling I had during the beginning of lockdown and remembered the “mourning” phase I went through in saying goodbye to the normal routine I had and prepared for the social, economic, and personal changes that were about to happen. This process changed my social routine, the way I interact with others, and the relationship I have with myself in ways that I didn't come to realize until being put back into a situation without the restrictions I had grown comfortable with. Having the psychological tools to ground yourself during moments of instability can make this journey all the more manageable. Unfortunately, we still have a long way to go. The next psychological phases have yet to present themselves, but they are surely going to change the way we live in a post-pandemic world. Looking at this time as an opportunity for growth and exploration is a comforting truth. We can all look to therapeutic techniques to support ourselves and each other. Sources: American Psychological Association (2021, March 11). Stress in America 2021 One Year Later, a New Wave of Pandemic Health Concerns. American Psychological Association. https://www.apa.org/news/press/releases/stress/2021/one-year-pandemic-stress Arlin, C. (2021, March 23). The Use of Acceptance and Commitment Therapy in Treating SAD. VerywellMind. https://www.verywellmind.com/acceptance-and-commitment-therapy-for-social-anxiety-3024910 Centers for Disease Control and Prevention. (2021, March 23). About CDC Covid-19 Data. Center for Disease Control and Prevention. https://www.cdc.gov/coronavirus/2019-ncov/covid-data/about-us-cases-deaths.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fcases-updates%2Fabout-us-cases-deaths.html Czeisler MÉ , Lane RI, Petrosky E, et al. Mental Health, Substance Use, and Suicidal Ideation During the COVID-19 Pandemic — United States, June 24–30, 2020. MMWR Morb Mortal Wkly Rep 2020;69:1049–1057. DOI: http://dx.doi.org/10.15585/mmwr.mm6932a1external icon. American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. Arlington, VA, American Psychiatric Association, 2013.
HOW TO HONOR THE INDIVIDUALS IN THE RELATIONSHIP THROUGH ATTACHMENT STYLES AND LOVE LANGUAGES12/18/2020 Author: Angellynn Lily Tam The words relationships and love are words heard throughout one’s lifetime. Often, the image that pops into our heads are scenes from movies, tv shows, and other media. The media’s portrayal of relationships has become our standard of what relationships and love are supposed to look and be like. We assume we find the one and live happily ever after. In actuality, relationships take work, but prior to working on the relationship as a couple, we first have to shift our focus and attention to acknowledge the two individuals that are in the relationship. We often forget that before getting into a relationship, we were once individual people who have decided to come together. In Dr. Keith Sutton's workshop for clinicians on Integrative Emotionally-Focused Couples Training, he teaches that we can honor the two individuals that choose to come together into a relationship by examining each person as their own part of the relationship. Each individual brings something unique to the table, and in order for a couple to work, we have to first understand each person and how each person shows and receives love. The first real connections we have are with our caregivers. As children, we are like sponges that soak up information all around us, even if we aren’t fully aware. The household in which we grow up plays a huge part in how one might show love to their significant other. The attachment styles one has are based on what we experience as children, primarily from our caregivers. If a child grew up around a parent who is abusive, that child may learn that it is normal behavior. This pattern of learnt behavior may continue into romantic relationships if it is not addressed. Identifying the characteristics of what is a healthy relationship versus unhealthy relationship are not taught, but learnt through observations and experiences. There are four different types of attachment styles: secure, anxious, avoidant-dismissive, and avoidant-fearful. Individuals with a secure attachment style are attuned with their emotions and are able to foster a safe, honest environment with their partners to speak out about upsetting topics. Individuals with anxious attachment style tend to struggle with their sense of self and romanticize about love with a positive view of their partner. Individuals with avoidant-dismissive attachment are emotionally distant from their partner and tend to suppress their feelings. Lastly, individuals with avoidant-fearful attachment style experience inner fluctuation of fear in being too close or too distant from their partners, which can lead to the relationship being volatile. It is important to note an individual’s attachment style when discussing behaviors within a relationship. Concurrent with attachment styles, it is also helpful to know individuals’ love languages. The different types of love languages are quality time, words of affirmation, receiving gifts, acts of service, and physical touch. Our love languages are how we tend to give, and wish to receive love. Knowing your partner's love language can help in understanding how to your partner shows love, and how to show love to your partner, and communicate how your partner can show love to you. So what does a healthy relationship look like compared to an unhealthy relationship? A healthy relationship is built around honesty, trust, mutual respect, and good communication. Self-esteem and self-confidence play a huge role in creating a safe space for both partners to be able to express their thoughts without judgement. There are many characteristics of an unhealthy relationship, but the main identifier of an unhealthy relationship is when one partner has more power over the other. This can lead to a potentially abusive relationship. With Emotionally Focused Couples Therapy (EFT), the focus is to develop the skills to be able to develop a secure attachment with their partner. This happens through understanding the cycle that gets in the way of each being able to communicate their love and care, and to be able to be responsive to each other. Often each partner loves their partner, and wants to connect, but the way that each tries to reach the other one, they end up missing each other. Relationships are not like in the movies, where they're all romance all the time and easy, but instead, it takes work to create a relationship that is fulfilling to each of the individuals, and make it the best relationship it can be. Through working on understanding our partners needs, our needs, and learning how to catch the cycle, we can strengthen our attachment bond, and have a relationship with a secure attachment, which is the foundation of true love.
Author: Milena Glasbeek Paul Chaudhuri Having a conversation about your mental health with another person can be challenging. Currently, physical health and mental health are not treated the same, especially in Western society. The existing stigma regarding mental health and the discrimination which often occurs, has created a significant barrier for people to seek help. Opening up to someone about your mental health struggles can lead to anxiety, feelings of shame, and uncertainty. You may wonder what the consequences of your disclosure will be, and how you will be perceived from that moment forward. Maybe you have already been speaking with a mental health professional and received a diagnosis, but have been keeping this a secret until now. Whether you have already spoken to a counselor, or if you will be speaking to someone about your mental health for the first time, taking the time to prepare for this delicate conversation can be an important first step. You can ask yourself the following questions in order to take charge of the conversation: 1. Why do I want to talk about my mental health? There could be various reasons why you have decided to speak about your mental illness or about seeing a mental health professional. People in your environment may have noticed a change in your mood or behavior. They might be asking questions and this could be the right time for you to answer them on your own terms. Sometimes it can be a relief to be able to share what you are going through with people close to you or with others in a similar situation who may be able to provide support. 2. What are my expectations? It is important to become aware of your expectations from the conversation. It is possible that the person you decide to talk to does not understand what you are going through, or reacts in a way that is not helpful to you. It may be tempting to stop talking about your mental health entirely if your expectations are not met. However, just because one person is not supportive does not mean that there may not be other people who could be of more help to you. 3. Who do I tell? How much do I tell? Since details regarding your mental health are private information, it is fully up to you to decide who you feel comfortable talking with and how much you would like to disclose. Think about who you trust, who would be understanding, and able to help you. When we have boundaries, we decide who we let in, and who we keep at an arm's distance. Ideally, those we let in should be people we trust, and have given us reason to feel safe with them. It may be useful to write down in advance what you would like to say. This could include:
Depending on the person you are speaking with, the conversation may look different. Here are some examples: 1. Sharing with a parent Not all parents are equally informed about mental health issues. The range of reactions that can be expected is guilt, concern, fear, relief, confusion, and more. They may need some time to process and could have many questions. 2. Sharing with a colleague or boss This situation can be complicated. You may want to keep the information you share limited. It could be enough to say: “I am experiencing some personal struggles, I would appreciate some flexibility/time-off/extra time, etc.” Or, if you need to get time off to go to therapy, you can say, "I've got a health issue where I'll need to go to a weekly meeting. I'll make up the time missed by coming in early that day". You don't have to discuss what is going on if you are concerned that it will lead to a negative perspective on your work performance. On the other hand, most everyone has struggled in their life, so explaining that you're going through a difficult time and getting help can help your boss make sense of recent work mistakes, as well as be assured you're addressing the issue. 3. Sharing with a friend Think about the pros and cons of speaking with a close friend versus a less close friend. Some people worry that their friendship will change, and that they will be perceived as a burden if they speak about their mental health struggles. On the other side, a friend who knows you well may be more compassionate, supportive, and ready to help. It is important to note that despite good intentions, friends might respond in ways that are insensitive or give unwanted advice. Therefore, take some time to consider which friend would be most able to give you the help you need and what the consequences could be for your friendship. 4. Sharing with a teacher or school counselor Many schools and colleges provide students with a counselor or contact person. Teachers and school counselors may have limited capability to give you long-term help, however, they may be a good point of contact for further resources and guidance on how to connect with a mental health care provider. 5. Sharing with a physician When people experience mental health-related issues, they often reach out to their primary care physician instead of contacting a mental health professional directly. PCP’s provide mental health care services such as diagnosis and (medical) treatment. Although primary care physicians have a general capability to provide mental health services, their consultation sessions are shorter compared to a psychotherapy session. Furthermore, PCP’s do not have the extensive training that mental health professionals have. Therefore, your primary care physician can help direct you to a mental health care professional if you decide to seek specialized care. 6. Sharing with a helpline Consider calling or texting a mental health helpline for free and confidential support. Crisis hotlines do not only provide suicide prevention services, they also provide support for people who are experiencing mental health struggles or going through a difficult time. Furthermore, they can provide you with information on resources through referrals to mental health care providers. Finally, consider preparing for this conversation with the help of a counselor or therapist. If you have been going to therapy you could ask your counselor to dedicate a therapy session to prepare for having the conversation about your mental health. Have you not yet spoken to a mental health professional? Therapy can be a safe space for you to share your experience without being judged and with a trained counselor who is willing to help. It is important to not be alone with your struggles, and whether talking to a therapist, a family member, a friend, or even calling a helpline to speak with an anonymous stranger, not being alone in your head with your difficulties is important. We are social creatures by nature and seek connection. Research has found that loneliness is one of the number one factors for not living a long life. When we can share our vulnerable parts with loved ones, often it signals empathy and for them to connect with us. For many it might lead them to worry, and feel like they have to fix it. Letting the person know you're having a hard time, but dealing with it through therapy, or working with a doctor can relieve the other person of feeling overwhelmed with wanting to help, and provide space for them to be supportive of you. Additional resources: National Suicide Prevention Lifeline: https://suicidepreventionlifeline.org Sources: Mental Illness Stigma and Disclosure: Consequences of Coming out of the Closet Understanding the impact of stigma on people with mental illness
The change from doing most of therapy in person to doing all of therapy remotely has been a big shock for both clients and clinicians. Many clinicians have never had to do video sessions, and have had to step out of their comfort zone and figure it out so they can be there for their clients during this time of need. Clients had to transition from the comfort of their therapists' office to doing therapy in sometimes not so comfortable places (e.g. home, car). Fortunately, doing therapy remotely also has its upsides. 1) Flexibility Doing therapy remotely has created a great deal of flexibility for clients who no longer have to drive to the office and juggle multiple work, child, and family obligations to carve out time to focus on their own self improvement. Although it can be a little harder with kids at home or having others in the house, the tradeoff of being able to see therapists during a lunch break or in the morning has made it easier for clients to get the help they've been needing. 2) Opportunity Let's consider the things that often hold people back from committing to therapy: the therapists office is too far away, they don't want to take time off of work, the social stigma of talking to their manager about taking time off of work to go, family commitments, etc. Now with the ability to do virtual sessions people may find themselves more open to the idea of taking time out of their lives to better themselves. Thanks to the flexibility of virtual sessions, clients are able to streamline getting help. Clients are able to begin the process of meeting therapists in a more efficient way, without having to leave their homes or find a day with no soccer practice to bring their child into therapy . Working remotely also allows them to manage some of the anxiety about talking to a stranger about the problems they've been struggling with. Lastly, for better or for worse, many problems that individuals, families, and couples have been dealing with have come to a head now that they are stuck at home. It was much easier to avoid the problems, but now many of those problems have been exacerbated, creating a crisis, and an opportunity to do something about it. 3) Connection via Screens Many therapists, as well as clients prefer to meet in person, feeling as though meeting remotely doesn't give the same human connection. It's true, you can feel the emotion in the room, and the connection when your therapist is really getting you, not just on an intellectual level, but what we feel inside. I've been doing therapy remotely for over 10 years, although they are usually one off sessions if a client is traveling, sick, etc. and it has been very effective. I was wary about starting with new individuals, families, and couples that I had never met in person, but I found that we were able to make a strong connection just as if we had met in person. While in-person sessions may be ideal, being able to connect with my clients through a screen while making them feel seen, heard, and attuned to has not been an issue. Whether I'm working with a couple in crisis, a teenager frustrated with their parents, a family and their anxious child, or an adult struggling with depression and ADHD, we're able to connect just the same as if we were working in person. 4) Move Forwards or Backwards We can either move forwards or backwards, but usually cannot stay stationary. Life continues to move on, and as they say in drug and alcohol counseling, "we are either moving towards our recovery or our relapse". This is a time to move towards your recovery, rather than letting problems snowball. Many families I have worked with who have struggled to develop structure with their children are now forced into a scenario where they have to figure it out. To work, do homeschooling, and keep children entertained day in and day out is hard, and its created the need to stop procrastinating and find a system that works. Many couples I've worked with were able to go through the motions, avoid each other in the time between getting home from work and going to bed. However, being stuck at home has forced them to turn to each other, to fight and resolve arguments, and find a resource in one another that they were able to survive without before. Several of the couples I work with have had to depend more on their relationship during this time, and have jumped into creating a more satisfying relationship for both partners. Many adults I work with have begun to address the issues they may have been avoiding such as connecting with friends and family, finally facing their anxieties about their finances, starting to exercise, and setting goals that work with family. This time of shelter in place and social distancing for many is creating a context where we can no longer avoid, and so choose to move forward, rather than backwards. 5) Accessing Expertise Finally, one of the biggest shifts of working remotely has been clients beginning to realize that distance doesn't matter, and they can get the expertise they've been needing. By removing the psychological barrier of needing to meet in person, clients are beginning to reach out from areas far away and finally work with someone who is trained to treat their specific problem. Whether it be exposure and response prevention for OCD, EMDR for PTSD, family therapy for oppositional defiance disorder, Cognitive Behavioral Therapy for adult ADHD, or Emotionally Focused Couples Therapy for relationship and sex problems, clients are finally getting specialized assistance, rather than transitioning from therapist to therapist who has a generalist approach. When working with an expert they're no longer talking about how their week was and just giving updates, but specifically addressing the problems they're dealing with and learning the tools to overcome their difficulties to create lasting change. There are many out there who are struggling, and many where things have gotten worse with their drinking or conflict at home, or loneliness becoming overwhelming, but with the help of a good therapist, this time in life can become an opportunity to move forward, rather than move backwards. The majority of therapists I speak with have been experiencing great success in their work with clients, and are often surprised at how the difference between working in person and remotely is not as great as they had thought. It's allowed people who have not been making progress in therapy to get the expertise they needed to create lasting change, and to everyone's surprise, a remote connection is still a strong and deep connection. I applaud the therapists who are becoming flexible and creative to provide what their clients need during this time of shelter in place, and encourage clients to reach out and take this opportunity to make the change they've been knowing they've been needing to make!  W. Keith Sutton, Psy.D. is the director of the Institute for the Advancement of Psychotherapy (www.sfiap.com) in San Francisco where he provides effective, evidence based treatments such as Structural-Strategic Family Therapy, Cognitive Behavioral Therapy (CBT), Emotionally Focused Couples Therapy (EFT), and Eye Movement Desensitization Reprocessing (EMDR). Dr. Sutton has expertise in children, adolescents, families, couples, and individual adults. He treats issues such as ADHD, OCD, depression, PTSD, panic attacks, anxiety, substance abuse/addiction, oppositional defiance disorder, relationship problems, and self harm. He also provides training through his Institute to licensed and prelicensed clinicians, and is the director of the nonprofit, Bay Area Community Counseling (www.sf-bacc.org), where he trains and supervises interns learning effective therapies and seeing clients in financial need. Dr. Sutton is the past president of the Association of Family Therapists of Northern California (www.aftnc.org) and the founder of Bay Area Therapists Specializing in Adolescents (www.batsa.net). |
Archives
October 2021
Categories |
- Home
- For Clients
-
For Professionals
- All Trainings
- On Demand Workshops
- Attachment Based - CBST Yearlong
- Summer Intensive
- One Way Mirror Training
- Consultation Groups
- CBT Training
- EFT Couples Training
- Family Therapy Training
- ESSFT Certification
- EMDR Training
- Child Therapy
- Motivational Interviewing
- ADHD Treatment
- Seeing the Blind Spots: A Consultation Group for Examining White Therapists' Privilege
- Seeing the Blind Spots: Exploring How You Think About and Experience Gender Diversity
- Supervision, Law, and Ethics
- Telehealth Workshop
- DBT for Alcohol and Drug Addiction
- Strength Based Culturally Informed Integrative Therapy
- About
- Contact
















 RSS Feed
RSS Feed